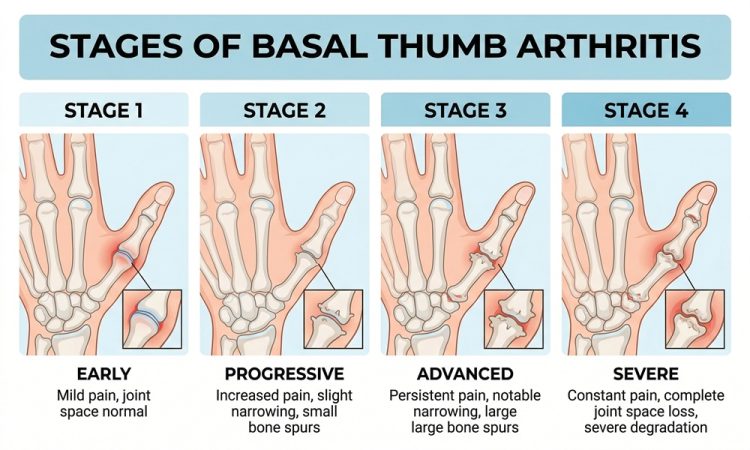
Basal thumb arthritis — also called basal joint arthritis or carpometacarpal (CMC) joint osteoarthritis — is one of the most functionally disabling forms of hand arthritis. While it may begin as a dull ache when you grip a jar or turn a key, it can progress into chronic pain, visible joint deformity, and significant loss of hand function. Understanding the stages of this condition is essential — both for timely diagnosis and for choosing the right treatment approach at the right time.
What Is Basal Thumb Arthritis?
The base of the thumb contains the carpometacarpal (CMC) joint, a saddle-shaped structure that connects the first metacarpal bone to the trapezium bone of the wrist. This joint allows the wide range of thumb movement we rely on daily — gripping, pinching, writing, and countless fine motor tasks.
Because of its unique biomechanics, the CMC joint bears enormous mechanical stress. Research shows that pinch force is amplified approximately 13 times within the basal joint, making it highly susceptible to cartilage wear over time. When this protective cartilage breaks down, the result is basal thumb arthritis — a progressive form of osteoarthritis that becomes increasingly common with age.
Who Is Most at Risk?
- Women over 50, particularly postmenopausal women — prevalence reaches up to 33% in this group
- Individuals over 30 years old in general — affecting up to 15% of this population
- People with a history of thumb ligament injury or joint laxity
- Those with occupations or hobbies requiring repetitive pinch gripping
The Eaton-Littler Classification: How Staging Works
The most widely accepted system for staging basal thumb arthritis is the Eaton and Littler (later Eaton and Glickel) Classification, which divides the condition into four progressive stages based on X-ray findings, joint space changes, osteophyte formation, and involvement of neighboring joints.
Important note: Radiographic stage does not always correlate directly with pain severity. Some patients with advanced X-ray changes report manageable symptoms, while others with early-stage findings experience significant functional disability.
The Four Stages of Basal Thumb Arthritis
Stage I — Early Joint Changes
What’s happening: The CMC joint may appear nearly normal on X-ray, but subtle widening of the joint space is visible — typically due to synovitis (joint lining inflammation) or early ligament laxity. Cartilage is still largely intact, but the volar beak ligament (the primary stabilizer of the joint) may begin to show signs of stress or early injury.
Symptoms at this stage:
- Aching pain at the base of the thumb, especially with activity
- Pain with forceful pinch or grip (opening jars, turning keys)
- Mild swelling around the CMC joint
- Occasional tenderness with direct pressure
Radiographic findings: Joint space appears normal or slightly widened; no significant osteophytes; possible joint laxity on stress views.
Stage II — Mild to Moderate Degeneration
What’s happening: Joint space begins to narrow, and the first small osteophytes (bone spurs) appear — typically less than 2 mm in size. There may be some joint debris present. Subluxation (partial dislocation) of the first metacarpal on the trapezium can often be demonstrated with specialized stress X-rays.
Symptoms at this stage:
- More persistent pain, present even with light activities
- Noticeable weakness in grip and pinch strength
- Swelling that may be visible at the base of the thumb
- Possible crepitus (cracking or grinding sensation during thumb movement)
Radiographic findings: Mild joint space narrowing, osteophytes < 2 mm, possible joint debris, subluxation on stress views.
Stage III — Significant Joint Destruction
What’s happening: Joint space narrowing becomes more pronounced. Osteophytes grow larger — exceeding 2 mm — and joint debris is more evident. The thumb metacarpal may show dorsal subluxation (the bone shifts out of position), which can create a visible “bump” or prominence at the base of the thumb. Surrounding soft tissue often becomes increasingly inflamed.
Symptoms at this stage:
- Pain present even at rest
- Significant stiffness, especially in the morning
- Visible deformity at the thumb base (dorsal prominence or “hump” sign)
- Marked reduction in grip and pinch strength
- Difficulty with daily activities such as writing, buttoning clothes, and opening containers
- Positive grind test on clinical examination (pain with axial compression and circumduction of the thumb)
Radiographic findings: Marked joint space narrowing, osteophytes > 2 mm, subchondral cysts, dorsal subluxation, sclerosis.
Stage IV — Advanced Disease with Pantrapezial Involvement
What’s happening: In the most advanced stage, the arthritis extends beyond the CMC joint to involve the scaphotrapezial joint (between the scaphoid and trapezium bones). This is sometimes called “pantrapezial arthritis.” The joint space is severely reduced or completely lost, and structural deformity of the thumb column is well established.
Symptoms at this stage:
- Chronic, often constant pain
- Severe functional limitation — even light touch may be painful
- Fixed deformity of the thumb (adduction contracture, MCP hyperextension)
- Significant muscle wasting around the thenar eminence
- Near-complete loss of thumb opposition and pinch grip
Radiographic findings: Complete or near-complete loss of joint space, large osteophytes, subchondral cysts and sclerosis, involvement of the scaphotrapezial joint.
Stage-by-Stage Summary Table
| Stage | Joint Space | Osteophytes | Subluxation | Scaphotrapezial Involvement | Primary Symptoms |
|---|---|---|---|---|---|
| I | Normal/slightly widened | None | Possible (stress views) | No | Activity-related pain, mild swelling |
| II | Mildly narrowed | < 2 mm | Yes | No | Persistent pain, grip weakness |
| III | Markedly narrowed | > 2 mm | Yes (dorsal) | No | Resting pain, visible deformity, stiffness |
| IV | Severely narrowed / lost | Large | Severe | Yes | Constant pain, fixed deformity, muscle wasting |
How Is Basal Thumb Arthritis Diagnosed?
Diagnosis is primarily clinical, supported by imaging.
Clinical Examination
A physician will assess for several hallmark signs:
- Grind test: Axial compression of the thumb combined with circumduction — pain and crepitus indicate CMC joint involvement
- “Hump” sign: Visible dorsal prominence due to metacarpal subluxation
- Point tenderness: Localized pain directly over the CMC joint
- Pinch and grip weakness: Measurable with a dynamometer
Imaging
X-rays remain the gold standard for diagnosis and staging. The ideal views include:
- Posteroanterior (PA) view of the hand
- True anteroposterior (Roberts view) of the thumb
- True lateral (Betts view) of the thumb
- Basal joint stress views for detecting early subluxation
MRI, CT, and ultrasound are not routinely required for basal thumb arthritis diagnosis or staging, though they may be used to rule out other conditions.
Conditions to Rule Out
Basal thumb arthritis can mimic or coexist with several other conditions:
- De Quervain’s tenosynovitis — tendon inflammation on the thumb side of the wrist
- Carpal tunnel syndrome — which coexists in up to 43% of patients with basal joint arthritis
- Scaphotrapezial arthritis
- Trigger thumb
- Metacarpophalangeal (MCP) joint arthritis
Treatment by Stage
Treatment strategy is closely tied to disease stage, though individual factors — age, activity demands, symptom severity, and response to conservative care — all influence decision-making.
Conservative (Non-Surgical) Treatment
Recommended as the first-line approach for all stages, conservative management focuses on offloading the CMC joint, reducing inflammation, and maintaining function.
| Treatment | How It Helps | Best For |
|---|---|---|
| Splinting / Orthoses | Stabilizes the CMC joint, reduces load during activity | All stages |
| NSAIDs (oral or topical) | Reduces inflammation and pain | Stages I–III |
| Corticosteroid injections | Temporarily relieves inflammation | Stages I–III (less effective in Stage IV) |
| Hand therapy / exercises | Improves joint mobility and surrounding muscle strength | All stages |
| Activity modification | Reduces mechanical stress on the joint | All stages |
| Ergonomic aids | Wide-grip tools reduce pinch force on the CMC joint | All stages |
Clinical insight: A 2004 randomized controlled trial found no significant clinical benefit of intra-articular corticosteroid injection over placebo in moderate to severe basal thumb arthritis — highlighting the importance of holistic conservative management rather than relying solely on injections.
Surgical Treatment
Surgery is considered when pain and functional loss persist after at least 6 months of consistent conservative treatment. The choice of surgical procedure is guided by the stage of arthritis and the patient’s lifestyle demands.
Early-Stage Procedures (Stages I–II)
These are joint-sparing approaches that aim to restore stability without removing bone:
- Ligament reconstruction: Rebuilding the volar beak or dorsal radial ligament to restore CMC joint stability
- Dorsoradial capsular imbrication: Tightening the joint capsule to reduce subluxation
- Extension osteotomy of the first metacarpal: Realigns the thumb to reduce joint stress
- CMC joint denervation: Interrupts pain signals from the joint
Late-Stage Procedures (Stages III–IV)
These are joint-sacrificing approaches for more advanced disease:
- Trapeziectomy: Removal of the trapezium bone, the most common surgical treatment for advanced basal thumb arthritis
- Trapeziectomy with LRTI (Ligament Reconstruction and Tendon Interposition): Removes the trapezium and uses a tendon graft to stabilize and cushion the space
- CMC joint fusion (arthrodesis): Permanently fuses the joint — offers strong pain relief but eliminates motion
- Total joint arthroplasty: Replaces the CMC joint with an implant — a growing option, particularly for active, younger patients
Living With Basal Thumb Arthritis: Practical Insights
Understanding your stage empowers better self-management. Here are evidence-based tips that apply across stages:
- Use wide-grip adaptive tools for kitchen utensils, pens, and door handles to reduce CMC joint load
- Wear a thumb spica splint during high-demand activities, even if symptoms are mild — early joint protection slows progression
- Avoid repetitive forceful pinch — lateral (key) pinch places the highest stress on the CMC joint
- Strengthen surrounding muscles — the abductor pollicis and thenar muscles help offload the joint when conditioned
- Maintain a healthy weight — systemic inflammation from obesity accelerates cartilage loss in all joints
- Seek early evaluation — patients who are diagnosed and treated in Stages I–II consistently achieve better long-term outcomes
When to See a Doctor
Do not delay consultation if you experience:
- Persistent thumb base pain lasting more than a few weeks
- Progressive weakness when gripping or pinching
- Visible swelling or a bump at the base of the thumb
- Pain that interrupts sleep or daily activities
- Sudden worsening of symptoms you’ve previously managed
Early intervention — particularly splinting and hand therapy — can significantly slow progression and delay or prevent the need for surgery.
Key Takeaways
- Basal thumb arthritis progresses through four defined stages (Eaton-Littler classification), from subtle joint widening to advanced pantrapezial involvement.
- It most commonly affects postmenopausal women, with up to 33% prevalence in this group.
- Radiographic stage does not always match symptom severity — clinical assessment matters as much as imaging.
- Conservative treatment — splinting, NSAIDs, therapy, and activity modification — is the foundation of management at every stage.
- Surgical options range from joint-preserving ligament reconstruction (early stages) to trapeziectomy (advanced stages), with good outcomes when matched to the right patient.
- Carpal tunnel syndrome coexists in up to 43% of cases — always worth screening for.