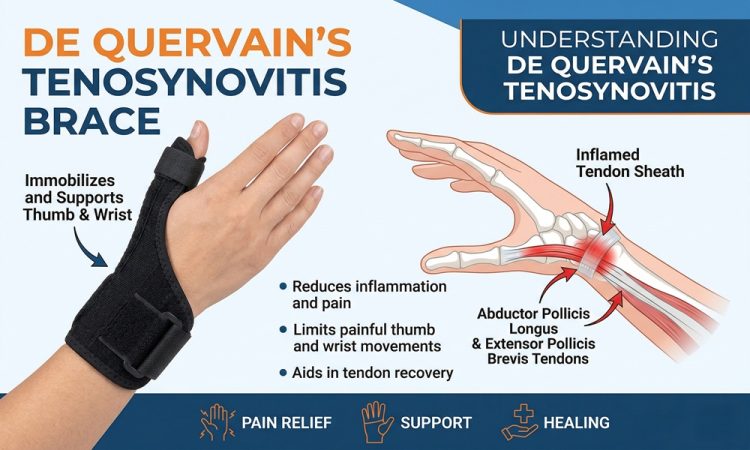
If you’ve ever felt a sharp, burning pain at the base of your thumb that worsens when you grip a coffee mug, pick up a child, or scroll on your phone — de Quervain’s tenosynovitis might be the culprit. And the first line of defence your doctor will likely recommend? A properly fitted brace.
This guide walks you through everything you need to know about de Quervain’s tenosynovitis braces: what they are, how they work, which type suits your situation, and how to use them effectively alongside other treatments.
What Is De Quervain’s Tenosynovitis?
De Quervain’s tenosynovitis (dQt) is a painful condition involving inflammation of the synovial sheaths surrounding two key tendons — the abductor pollicis longus (APL) and the extensor pollicis brevis (EPB) — as they pass through the first dorsal wrist compartment on the thumb side of your wrist.
The condition is commonly known by several nicknames that reflect its most frequent causes:
- Mommy Thumb — from repetitive infant lifting
- Texting Thumb — from prolonged smartphone use
- Gamer’s Thumb — from repetitive controller gripping
Women aged 40–60 are statistically more affected, but the condition is increasingly common in young adults due to heavy smart device use. It can affect anyone performing repetitive hand or wrist motions — from office workers and musicians to gardeners and new parents.
Common Symptoms
- Pain and tenderness along the thumb side of the wrist
- Swelling near the base of the thumb
- Difficulty gripping, pinching, or twisting the wrist
- A snapping or catching sensation when moving the thumb
- Pain that worsens with activity and improves with rest
A positive Finkelstein test (tucking the thumb inside a fist and bending the wrist toward the little finger) is the standard clinical diagnostic indicator, though the WHAT test (wrist hyperflexion and thumb abduction) offers greater specificity.
Why a Brace Is Central to Treatment
Bracing is one of the most recommended non-invasive, first-line treatments for de Quervain’s tenosynovitis. The rationale is straightforward: the inflamed tendons cannot heal if they continue to be stressed with every thumb and wrist movement. A properly fitted brace enforces the rest those tendons desperately need.
According to a 2024 systematic review and network meta-analysis published in JAMA Surgery, combining a corticosteroid injection with 3–4 weeks of thumb spica immobilization is associated with the best short-term pain relief and functional outcomes. Bracing alone — without injection — still offers meaningful relief for mild to moderate cases.
A brace for de Quervain’s works by:
- Immobilizing the thumb and wrist to prevent the APL and EPB tendons from being pulled repeatedly through the narrowed tendon sheath
- Reducing mechanical stress on inflamed tissue, allowing swelling to subside
- Providing mild compression to help manage local oedema
- Preventing unintentional nighttime movements that can re-aggravate healing tendons
Types of Braces for De Quervain’s Tenosynovitis
Not all braces are equal. Choosing the right type depends on the severity of your condition, your lifestyle, and how much daily hand function you need to preserve.
1. Thumb Spica Splint (Most Recommended)
The thumb spica splint is the gold standard for de Quervain’s. It immobilizes both the thumb and the wrist, leaving the fingers free. The term “spica” refers to the figure-8 wrapping pattern that anchors the thumb securely.
It comes in two sub-variants:
- Long thumb spica — extends further up the forearm for maximum immobilization; ideal for severe or post-injection cases
- Short thumb spica — covers just the wrist and thumb base; better for mild-to-moderate cases and daily wear
2. Cock-Up Wrist Splint with Thumb Extension
This design includes an ergonomic aluminum or thermoplastic stay that holds the wrist in slight extension (the “cock-up” position) while a separate spica extension secures the thumb. It immobilizes both the metacarpophalangeal (MCP) joint and the carpometacarpal (CMC) joint.
3. Fabric Compression Brace with Thumb Loop
A softer, semi-rigid option that wraps the wrist and passes a loop around the thumb. It offers lighter support and is best suited for:
- Mild symptoms
- Return-to-activity phase
- People who cannot fully restrict their hand use due to work demands
4. Custom-Molded Thermoplastic Splint
Made by a certified hand therapist, these are heat-shaped to fit the exact contours of your wrist and thumb. A 2024 study in Health Science Reports explored the role of 3D-printed personalized braces for stenosing tenosynovitis, showing improved pressure distribution and wear comfort over standard OTC options.
Brace Types at a Glance
| Brace Type | Support Level | Best For | Finger Freedom |
|---|---|---|---|
| Long Thumb Spica | High | Post-injection, severe cases | Full |
| Short Thumb Spica | Moderate–High | Mild to moderate dQt | Full |
| Cock-Up Wrist + Thumb | Moderate–High | Daily wear, MCP/CMC support | Full |
| Fabric Compression Brace | Mild–Moderate | Return-to-activity phase | Partial |
| Custom Thermoplastic Splint | Very High | Chronic or atypical cases | Full |
Key Features to Look for in a De Quervain’s Brace
When shopping for a brace — whether online or through a medical supplier — these are the features that matter most:
Structural Support
Look for removable aluminum or thermoplastic stays that can be shaped to your wrist’s natural curvature. A rigid spica that secures the thumb in a slightly abducted position is essential for true immobilization.
Breathability
Braces must be worn for weeks. Materials like perforated neoprene, breathable nylon, or hollow-mesh fabric prevent excessive heat buildup and skin irritation — a common reason people stop wearing their splints prematurely.
Adjustability
Velcro straps or contact-closure designs allow you to fine-tune the compression level. Avoid fixed-tension braces that cannot adapt to changing swelling throughout the day.
Ambidextrous vs. Hand-Specific
Many high-quality braces are hand-specific (left or right) to ensure anatomical fit. Ambidextrous models offer convenience but may compromise the contour and support precision.
Day and Night Suitability
Choose a lightweight, slim-profile brace that can be worn comfortably during sleep without causing pressure sores or overheating.
How to Wear Your Brace Correctly
Wearing the brace correctly is just as important as choosing the right one. Here is a practical guide:
Step 1 — Position the Wrist Stay Slide the metal or plastic stay along the palm-facing side of your wrist. The stay should extend from mid-forearm to just below the knuckles.
Step 2 — Secure the Thumb Spica Wrap the thumb portion so the thumb rests in a natural, slightly abducted position — not pulled tightly inward or forced outward. The interphalangeal (IP) joint of the thumb (the top thumb joint) is typically left free.
Step 3 — Fasten the Straps Secure from wrist upward. The brace should feel snug but not restrict blood flow. If your fingers tingle or turn pale, loosen the straps.
Step 4 — Check Your Finger Mobility Your index, middle, ring, and little fingers should move freely. The brace should not restrict finger flexion or extension.
When to wear it:
- During all waking hours in the acute phase
- Overnight to prevent unguarded movements
- During physical activity or work tasks involving hand use
When you can remove it:
- Bathing (unless instructed otherwise)
- Gentle range-of-motion exercises prescribed by a therapist
How Long Should You Wear a Brace?
The duration depends on symptom severity and whether you are combining bracing with other treatments.
| Severity / Treatment Stage | Typical Bracing Duration |
|---|---|
| Mild symptoms, brace only | 4–6 weeks |
| Moderate symptoms with NSAIDs | 4–6 weeks |
| Post-corticosteroid injection | 3–4 weeks (evidence-based) |
| Return-to-activity phase | As needed during demanding tasks |
| Recurrent or chronic cases | Ongoing use during flare-ups |
Most people need to wear a splint for at least a few weeks. Do not stop wearing the brace early just because pain has reduced — tendons need continued rest to fully remodel the inflamed tissue.
Brace vs. Other Treatments: Where Does It Fit?
A brace is almost never the sole treatment. Here’s how it fits into the broader management picture:
Conservative Treatment Ladder
Rest + Brace → NSAIDs → Corticosteroid Injection + Brace → Physical Therapy → Surgery (Last Resort)
Research consistently shows that corticosteroid injection combined with thumb spica immobilization produces superior short- to mid-term outcomes compared to bracing alone or injection alone for moderate-to-severe cases. Ultrasound-guided injection is associated with even greater pain reduction than conventional injection.
Physical therapy after the initial immobilization phase focuses on:
- Tendon gliding exercises
- Gradual strengthening of the wrist extensors
- Activity modification coaching
- Ergonomic adjustments
Surgery (first dorsal compartment release) is reserved for cases where conservative management fails over several months.
Practical Tips for Living With a De Quervain’s Brace
Managing daily life while wearing a splint requires some adjustment. These tips help you stay functional and consistent with your treatment:
- Modify your grip: Use two hands for lifting, or use assistive tools like jar openers to reduce thumb load
- Switch phone hands: Alternate which hand you use for texting; use voice-to-text when possible
- Keep a spare brace: Having a backup allows you to wash one while wearing the other
- Apply ice before putting on the brace: A 15–20 minute ice pack session before bracing helps reduce swelling and makes wear more comfortable
- Clean the brace regularly: Most fabric braces can be hand-washed in mild soap and air dried — check manufacturer instructions
- Mark your wrist: After removing the brace, look for red lines or pressure marks. Reposition the straps if consistent pressure points develop
When to See a Doctor
A brace is an excellent starting point, but certain signs indicate you need a medical evaluation before or alongside bracing:
- Pain that is severe, constant, or worsening despite 2 weeks of bracing
- Significant visible swelling or warmth over the radial wrist
- Numbness or tingling in the thumb or fingers
- Symptoms that began after a direct injury or fall
- No improvement after 4–6 weeks of conservative care
A healthcare provider may order an ultrasound to confirm tendon sheath thickening or rule out other conditions such as intersection syndrome, carpal tunnel syndrome, or basal joint arthritis — all of which can mimic de Quervain’s.
Final Thoughts
A de Quervain’s tenosynovitis brace — particularly a thumb spica splint — is one of the most effective and accessible tools in recovering from this painful condition. The key is choosing the right type for your severity, wearing it consistently (day and night during the acute phase), and pairing it with appropriate complementary care such as rest, ice, NSAIDs, or a corticosteroid injection if recommended by your provider.
The condition is very treatable. With the right brace, proper use, and a little patience, most people return to full pain-free function within a few weeks to a couple of months. The worst thing you can do is wear the brace inconsistently or abandon it the moment pain starts to ease — that is precisely when the tendons are most vulnerable to re-injury.
Invest in a well-fitting, breathable, medically appropriate splint, follow your provider’s guidance on duration, and give your tendons the recovery window they need.